The patellar tendon is a strong band of tissue responsible for keeping the kneecap in place, stabilizing the knee, and enabling movements like jumping, running, and squatting. Despite how reliable and resilient this tendon is, overuse and the age-related degeneration of tissue can lead to what’s known as “jumper’s knee” – an inflammatory condition that causes pain and restricted mobility.
Fortunately, taking medications daily to manage the pain or undergoing invasive surgical procedures are no longer the only options if you have patellar tendonitis. In this guide, we’ll explore how Neuragenex Neurofunctional Pain Management can help you regain your knee health without surgery or drugs.
Let’s get started.
What Is Patellar Tendon Pain?
Patellar tendonitis or tendinopathy is a condition defined by the inflammation and damage of the patellar tendon. The patellar tendon is a strong band of tissue that connects the bottom of the patella (the kneecap) to the top of the shinbone (tibia). Although it is referred to as a “tendon”, this cord of tissue is, in fact, a ligament, as it connects two bones.
Its main role is to provide stability and range of motion to the knee, as well as prevent injuries like dislocations during jumping and squatting movements. The patellar tendon also works together with the surrounding muscles to enable the movement that allows you to bend and straighten the knee.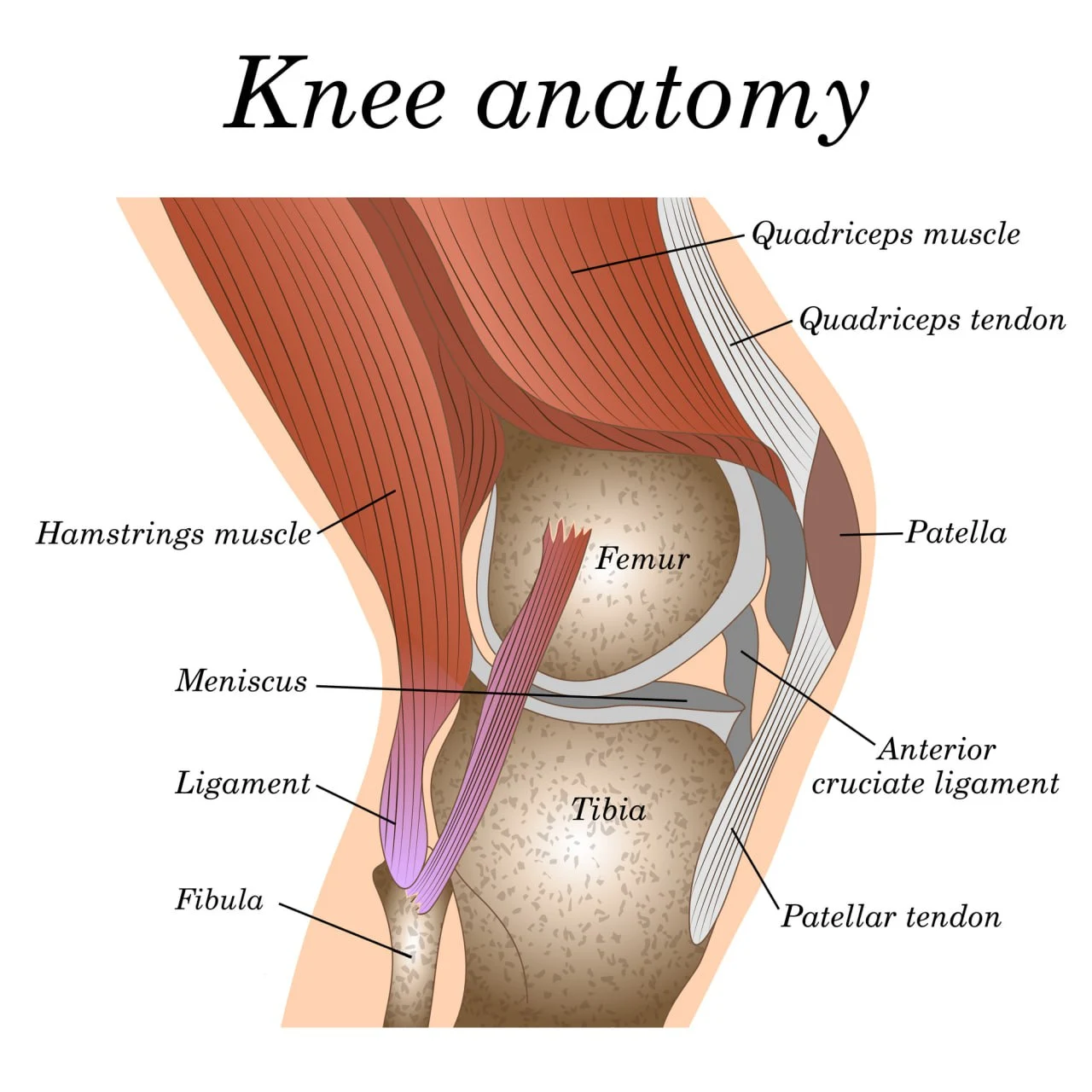
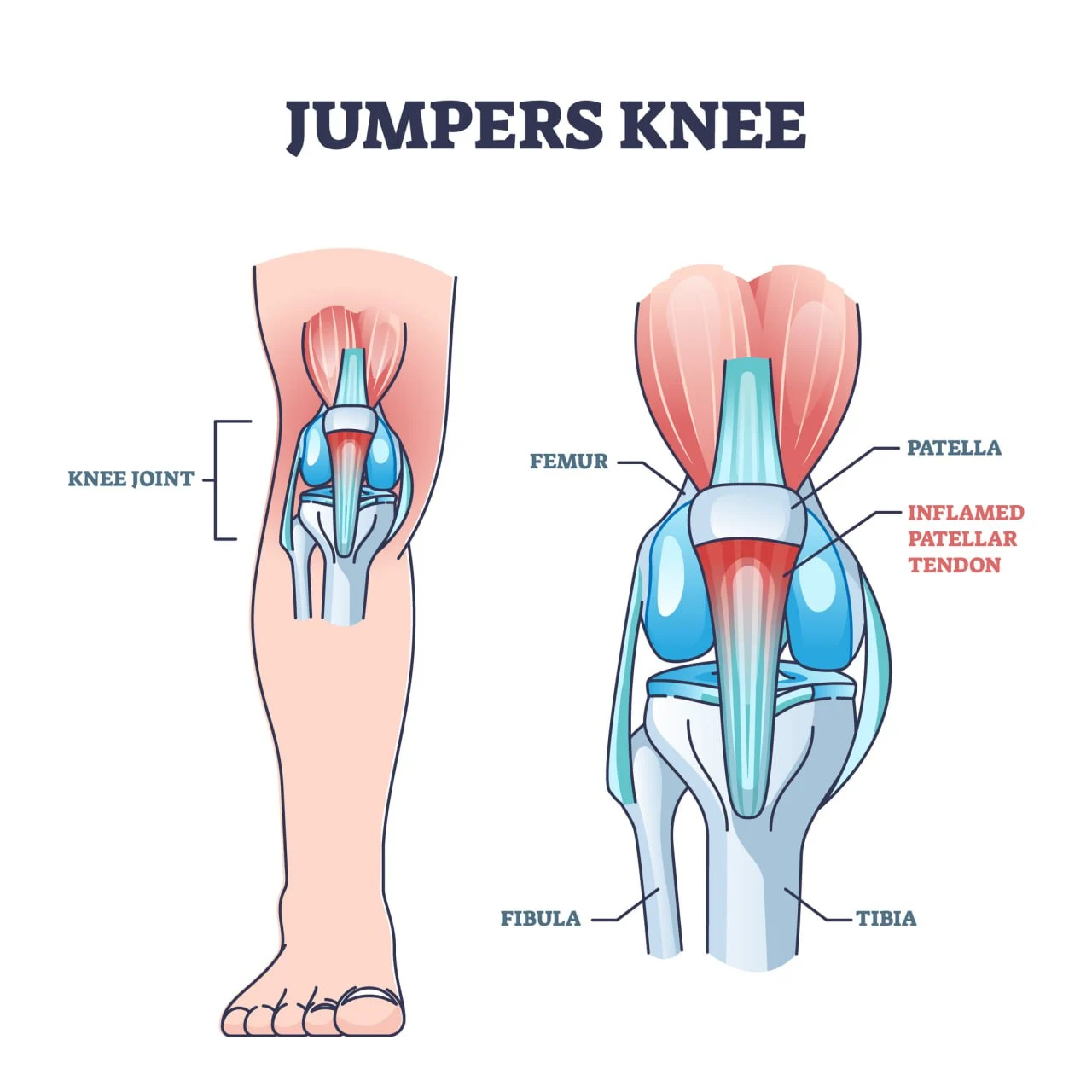
Patellar tendonitis occurs when the patellar tendon becomes irritated, torn, inflamed, or damaged due to overuse, stress, or tissue degeneration. This condition causes severe pain and restricted mobility, which can prevent you from participating in sports and competitions.
Given that over 45% of jumping athletes and up to 14% of recreational jumping athletes will experience patellar tendonitis during their careers, this condition is often dubbed “jumper’s knee”.
The level of pain caused by this condition varies, with some people only experiencing mild discomfort and others struggling with chronic pain. When left unaddressed, a knee affected by patellar tendonitis can take months to heal fully.
In the sections below, we’ll explore what patellar tendon pain feels like, what causes it, and how you can address it efficiently without surgery or medications.
How Does Pain In The Patellar Tendon Feel?

Patellar tendonitis occurs over time, often due to repeated stress to the knee or excessive load bearing. This means that, at first, you may only experience minor discomfort around the knee. However, when left untreated, mild knee discomfort can develop into severe, life-limiting pain.
Because of the pain and swelling, you may become unable to perform daily activities that involve bending the knee (e.g. climbing stairs, sitting, and squatting). If you are an athlete or sportsperson, the pain may intensify during physical activity and prevent you from participating in sports.
Some of the key symptoms that may indicate patellar tendonitis include:
- Pain under the kneecap, where it connects to the shinbone. Patellar tendon pain can appear as a dull ache that worsens over time and during physical activity.
- Difficulty fully extending the knee. Inflammation around the patellar tendon often causes swelling and stiffness. These complications occur as part of the normal inflammatory response of the body, which increases blood circulation and causes the build-up of fluids around the site of injury. The stiffness, coupled with pain and swelling, can prevent you from fully straightening the knee.
- Increased pain during specific movements. Patellar tendonitis often manifests itself as pain that intensifies during knee motion that involves the patellar tendon. These motions include jumping, squatting, and descending stairs.
Common Places Where The Pain Is Felt
If you experience pain around the knee, it is important to understand whether this is related to problems with the patellar tendon, or whether other structures are involved (i.e. the cruciate or lateral ligaments).
An easy way to self-diagnose patellar tendonitis is to assess where the pain is located. You may suffer from this condition if:
- You experience pain below the kneecap, at the top of the shinbone.
- Swelling is present where the patellar tendon attaches to the shinbone, at the front of your knee.
- The area under your kneecap may feel tender or painful only when touching it.
- You experience burning sensations when bending your knee, jumping, or getting up from a squat.
Patellar Tendon Pain Causes and Risk Factors
Patellar tendon pain often develops as a consequence of overuse, excessive stress to the knee, or abnormal load bearing. However, it can also stem from other causes and risk factors, including aging, inflammatory conditions like arthritis, knee injuries, and chronic diseases that weaken the knee.
Next, we’ll explore the most common causes of patellar tendon pain.
Overuse or Repetitive Strain
The most common causes of patellar tendon pain are overuse and repetitive strain of the patellar tendon. When the tendon needs to withstand excessive stress for prolonged periods, it can become more prone to micro-tears and injuries, which reduce the supply of blood to the area and trigger the body’s inflammatory response (i.e. pain and swelling).
This can occur due to activities that involve the patellar tendon and put excessive strain on its tissues, such as jumping, sprinting, or changing direction at fast speeds.
So it isn’t surprising that patellar tendonitis is highly prevalent among recreational and elite athletes. For example, it is estimated that up to half of all professional volleyball players will struggle with patellar tendon pain during their careers. And, in most cases, patellar tendon pain becomes a recurring or chronic condition that significantly interferes with their performance.
The risk of developing patellar tendonitis as an athlete depends on multiple factors, including:
- Level of participation in sports that involve jumping motions
- Frequency of training
- Type of sport
Some of the activities that significantly increase the risk of patellar tendon pain include basketball, dance, football, gymnastics, running, volleyball, track, and figure skating.
Nonetheless, playing certain sports isn’t the only factor that can put your patellar tendon under excessive stress. For example, if you are overweight or obese, carrying excessive weight can strain the knee and cause constant stress to its components. According to a 2014 study, obesity is directly associated with a greater risk of patellar tendinopathy, and nearly 30% of patients with a high BMI (body mass index) report signs of jumper’s knee.
Previous Knee Injuries
Past knee injuries can have a profound impact on the overall health of your knee and increase your risk of suffering from patellar tendon pain. In particular, a 2008 study shows that a single traumatic event can lead to chronic patellar tendon problems and traumatic patellar tendinopathy.
Additionally, this condition can stem from old knee injuries due to:
- Improper rehabilitation or recovery
- Fractures that have changed the mechanics of the knee
- Misalignments and mechanical problems to the feet, ankles, and legs
These medical events can impact how the knee moves and how external forces are redistributed by load-bearing joints, thus adding abnormal pressure to the patellar tendon during movements.
Rheumatoid Arthritis
Rheumatoid arthritis is an inflammatory and autoimmune disease that occurs when the body’s immune system mistakenly attacks healthy cells and tissues, such as the ones in the knee joint. Rheumatoid arthritis causes sustained high levels of inflammation that, over time, cause the degeneration of essential structures like bones, ligaments, and tendons.
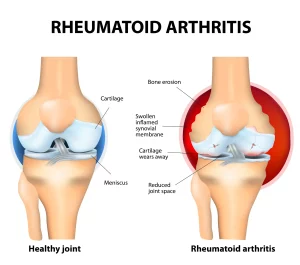
Patellar tendon pain in people with rheumatoid arthritis is caused by damage and tearing of the tendon, as well as changes in the mechanics of the knee, which occur when the joint components are severely damaged. According to another 2014 study, patellar tendon problems are among the leading causes of loss of lower limb function in those with rheumatoid arthritis.
Diabetes
Suffering from diabetes and uncontrolled blood sugar levels can lead to several changes in the structure of ligaments, especially in terms of thickness, flexibility, and healing capacity.
This occurs due to the advanced glycation end products (AGEs). AGEs are products that are formed in the body when certain proteins or fats combine with sugar in the blood. In healthy patients, AGEs are produced slowly and steadily, giving time for the body to process them. However, in people with diabetes, high levels of blood sugar speed up the production of AGEs, which begin to bind to and build up on the collagen fibers of tendons and ligaments.
The accumulation of these substances causes the patellar tendon to grow thicker and less flexible, which makes it unable to bear loads during movement. Over time, this can increase the risk of patellar tendon injuries and tears, which leads to ongoing pain and inflammation.
Age and Degeneration
As we age, the fibrous tissues around the body – including tendons and ligaments – begin to degenerate and lose flexibility. When this occurs in the knee, patellar tendon injuries and tears are more likely to happen, especially following a sudden or forceful movement.
In particular, those around the age of 40 are most at risk, because they may remain active and continue participating in sports, thus increasing the likelihood of battling knee injuries.
Existing Medical Conditions
Certain medical conditions and chronic illnesses tend to negatively impact bone health by inhibiting the supply of blood, oxygen, and nutrients to the knee and its components. Without adequate blood circulation, the fibers of tendons and ligaments become less flexible and supple, which increases the risk of injuries and speeds up the degeneration of tissues.
Some of the diseases that increase the risk of patellar tendon problems include kidney failure and dysfunction, diabetes, and autoimmune diseases such as lupus.
When To Seek Professional Help
Although mild knee discomfort may be a temporary condition that can be treated at home with conservative measures such as applying an ice pack, it is important to understand when to see a doctor. If left unaddressed, patellar tendon pain can develop into a life-limiting, debilitating disease – and, in severe cases, it can lead to severe complications such as the rupture (or complete tearing) of the patellar tendon.
Learning to assess when your condition requires medical attention is the first step to avoid further problems, invasive treatments, or permanent damage to the knee. Some of the telltale signs you should look out for include:
- Worsening of your pain after physical activity
- Pain and aching that last long after you stop an intense activity
- Severe knee pain that appears as burning or sharp sensations, especially after a sudden movement
- Pain that lasts more than two or three days
- Painful sensations and mobility issues that have started to interfere with your daily life
Diagnostic Procedures
Because of how complex the knee structure is, obtaining an accurate diagnosis that pinpoints the exact source and causes of your knee pain is of vital importance. That is why your healthcare provider will use a range of diagnostic tools, including:
- Physical examinations: Physical exams are used to determine the intensity, location, and nature of your symptoms. Your doctor will do so by asking direct questions, palpating the knee, and moving your leg slightly to check when or where it hurts. Your healthcare provider will also ask you about your activity levels and the sports you practice.
- Imaging tests: Although imaging tests are not always accurate when it comes to diagnosing tendon injuries, X-rays, MRIs, and ultrasound tests can be used to rule out other potential causes of pain, such as tumors and structural anomalies.
- Blood tests: Blood tests can help identify diseases that may be contributing to your knee pain, including diabetes and rheumatoid arthritis.
Electromyography (EMG) tests: EMG tests are used to assess the response of muscles and electrical activity. In the case of knee pain, they may be used to obtain information about an injury to muscles or nerves.
Common Treatment Options
Treating patellar tendon pain isn’t always straightforward, especially if the degeneration of the tendon is caused by chronic diseases like rheumatoid arthritis or diabetes. Most patients are prescribed pain medications, physical therapy, or corticosteroid injections.
Given how common patellar tendon pain is among athletes and adults of all ages, more clinical trials on the effectiveness of other treatments – such as the use of collagen and vitamin C for jumper’s knee – are being carried out. Nonetheless, today’s patients with chronic patellar tendon pain still live with the fear of having to undergo surgery.
In the sections below, we’ll look at the most common patellar tendon pain treatments.
Pain Medication
Over-the-counter pain medications are usually the first line of treatment for patellar pain. Medications such as ibuprofen (Advil), acetaminophen (Tylenol), and naproxen sodium (Aleve) can provide relief during pain flare-ups and allow you to carry out your daily activities.
Nonetheless, it is important to note that patellar tendon pain can last for months at a time, and, in most cases, it develops into a chronic, recurring condition. Taking pain medications daily for such extended stretches of time isn’t free of risk: pain medications and non-steroidal anti-inflammatory drugs (NSAIDs) cause a cascade of side effects, including a higher risk of heart attack and stroke, stomach ulcers, digestive issues, and addiction.
Physical Therapy
Physical therapy can help you reduce the symptoms associated with patellar tendonitis, including pain and inflammation. At the same time, targeted knee exercises may help increase the flexibility and strength of surrounding muscles, which play a vital role in improving overall knee health.
Common exercises you may practice with your therapist include:
- Stretching
- Warm-up exercises
- Massages
- Strength and resistance training
- Flexibility exercises to lengthen the calf muscles
- Isometric exercises, which involve holding the body in a certain position with no joint movement
According to a 2006 study, eccentric squats performed on a 25-degree decline board increase the strain of the patellar tendon, thus offering better results in terms of strength training and rehabilitation of patellar tendon problems.
Corticosteroid Injection
Corticosteroids are the synthetic version of chemicals that are naturally found in the body, which are responsible for regulating the transmission and processing of pain signals. Injected in the area around the patellar tendon, these drugs provide longer-lasting relief from severe pain.
Just like any other medication, corticosteroid injections come with considerable side effects that you should discuss with your doctor. In particular, according to a 2016 study, the spontaneous rupture of a tendon is a severe side effect of corticosteroid injections for tendonitis.
Patellar Tendon Strap or Brace
Using braces and clutches for a period of time while you are recovering from patellar tendonitis may help you relieve pressure on the knee joint and prevent further damage. This is especially the case if your injury is caused by overuse.

Braces and straps worn tightly around the knee also help reduce inflammation, pain, and swelling. Once the pain has eased, you will be able to start physical activity and rehabilitation.
Surgery
If none of the treatments above are successful in easing your patellar tendon pain, your doctor may recommend a surgical intervention to repair the patellar tendon.
Depending on the type of surgery, your doctor may need to open the knee to scrape and clean the different components affected by inflammation, including the kneecap and the patellar tendon. The injured part of the tendon may also be removed. Alternatively, a thin viewing instrument (arthroscope) may be inserted through a small incision in the knee area to carry out the same tasks with far less damage to surrounding structures.
In severe cases, a surgical procedure known as tenotomy can be used to cut through the tendon to disconnect it from the surrounding structures and allow for a greater range of motion. Another method is to realign the kneecap to relieve the tension on the patellar tendon.
Although over 10% of athletes with jumper’s knee undergo surgery for their condition, surgery should always be considered as the last resort. Firstly, surgical interventions involve between six weeks (for arthroscopic surgery) and four months of immobilization and rehabilitation.
Additionally, surgical interventions are never free of risks: an invasive procedure may permanently compromise your knee function, expose you to infections, and get in the way of your career as an athlete.
Neuragenex Neurofunctional Pain Management For Patellar Tendonitis
Although patellar tendon pain may seem like a minor issue at first, it can develop into a life-restricting condition that will continue to interfere with your personal, professional, and athletic career for years to come – if not treated properly.
However, enduring taking medications daily for months on end or fearing the need for invasive surgery are just some of the options in front of you today. Pioneered by Neuragenex, Neurofunctional Pain Management is a whole-person approach to treating pain conditions that do not involve drugs or invasive procedures.
With a structured Neuragenex Neurofunctional Pain Management designed around your unique needs, you can restore your musculoskeletal health, regain knee function, return to enjoying the activities you love the most, and live pain-free.

Below, we’ll explore the therapies that work as the main pillars of Neuragenex Neurofunctional Pain Management.
Electroanalgesia
Electroanalgesia is a pain management technique that uses high-pulse electrical current to ease pain, boost blood circulation, improve mobility, and induce...
IV Therapy
IV nutritional therapy, or intravenous therapy, involves administering vital nutrients directly to the bloodstream through an IV. This type of treatment bypasses the digestive system, allowing for maximum absorption and utilization of nutrients by the...
Lifestyle Counseling
Lifestyle counseling is an approach to managing chronic pain that involves identifying, assessing, and modifying lifestyle factors contributing to an individual's pain. For example, lifestyle factors such as nutrition, physical activity, stress, sleep quality...
Preventive Strategies
Although athletes run the highest risk of suffering from patellar tendon pain, this condition can affect anyone, at any age. Given the long-term impact it can have on your health, it is important to take steps to prevent it.
Some prevention tips that can help you include:
- Wear appropriate footwear – especially during exercise – to safeguard normal knee mechanics and alignments.
- Ensure adequate recovery time between training sessions.
- Ease down on exercise when you experience discomfort.
- Don’t play through pain – this can cause larger tears in the tendon and significantly aggravate your condition.
- Warm up and cool down properly.
- Avoid activities that put your knee under excessive stress.
- Strengthen the muscles that support the knee.
- Perfect your form and technique, especially when practicing sports at high levels.
- Maintain a healthy weight.
Get Relief From Pain
Not treating patellar tendon pain can cause you to live in pain through everyday activities and even put a stop to your career as an athlete. But fortunately, you can now access a customized Neuragenex Neurofunctional Pain Management program that can help you restore your health, relieve pain, and magnify your quality of life. And you can achieve all this without taking medications daily or undergoing surgery.
Get relief from patellar tendon pain today.




